Information on Ear Conditions
Cholesteatoma
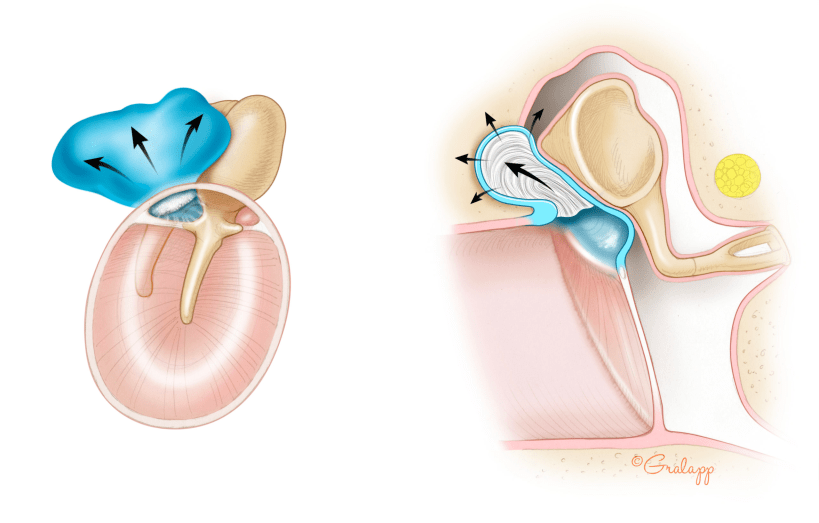
Cholesteatoma is a skin cyst that grows in the ear canal and/or middle ear. How cholesteatomas form is still not fully understood. It is thought to form from native ear canal skin that becomes trapped in a pocket, which can lead to inflammation and infection. The cyst continues to grow as more skin becomes trapped, and the inflammation and infection that ensues can cause destruction of middle ear structures and subsequent ear fullness, hearing loss, tinnitus, imbalance or vertigo. Cholesteatomas can be asymptomatic early on, but if they get infected, they cause foul-smelling ear drainage.
Cholesteatomas occur in 1 in 20,000 people, but it is a common condition we treat at Atlanta Otology. There are no medications that can treat cholesteatoma. The majority of cholesteatomas are best treated with surgical removal. If they are ignored, they can lead to very serious complications such as facial nerve paralysis, brain fluid leak, and brain infection. Cholesteatomas can be diagnosed by your ENT doctor through an otoscopic or microscopic exam. CT and/or MRI scans are often performed to evaluate the extent of disease.
Hearing loss
One in eight people in the United States aged 12 years or older have hearing loss in both ears, and 2 of every 1000 children in the United States are born with hearing loss. Hearing loss can cause major obstacles in life: it impairs learning ability in children, limits occupational opportunities, leads to social isolation, and contributes to depression. Helen Keller, a famous author who developed a severe illness as an infant that left her blind and deaf once said, “Blindness separates people from things, deafness separates people from people.”
There are many different forms of hearing loss: some that can be gradual and others that can be sudden, some that affect young people and others that affect older adults, and some that are due to mechanical issues and others that are a result of nerve problems. Our doctors at Atlanta Otology are specialists of the ear and auditory system and can evaluate and discuss options for your specific cause of hearing loss.
Acute otitis media
Acute otitis media (AOM) refers to an infection of the middle ear of acute onset. It is more common in children – more than 80% of children have at least one episode of AOM before they are 3 years old. Adults can also develop AOM, but less commonly. Risk factors for developing AOM include smoke exposure, family history of ear infections, poor immune system, upper respiratory infection, and (in children) exposure to daycare. AOM is thought to arise from an improperly working eustachian tube. In children, the orientation of the eustachian tube is more horizontal than that in adults, and prevents normal drainage of middle ear fluid. When the fluid is unable to drain, the fluid can become infected by bacteria. Patients with AOM typically develop ear pain, fever, and hearing loss. Sometimes, the pressure from the fluid in the middle ear causes an ear drum rupture and the patient will notice foul-smelling drainage. AOM is normally treated with oral antibiotics and sometimes antibiotic ear drops. AOM that keep recurring may require ear tubes.
Acute otitis externa (swimmer’s ear)
Acute otitis externa (AOE), or ‘swimmer’s ear’, refers to an infection of the ear canal. Symptoms include ear pain, ear drainage, and hearing loss. This condition occurs when bacteria or fungus grows in your ear canal, which can happen as a result of dirty water getting into your ear, eczema of the ear canal, prolonged use of hearing aids, or excessive ear cleaning. The condition can be diagnosed by your doctor with a physical examination. AOE is usually treated with antibiotic ear drops and sometimes oral antibiotics. If there is drainage in the ear, your doctor may culture the fluid. If there is a significant amount of swelling of the ear canal, your doctor may place an ear wick to allow the medication to work.
Vertigo/Dizziness
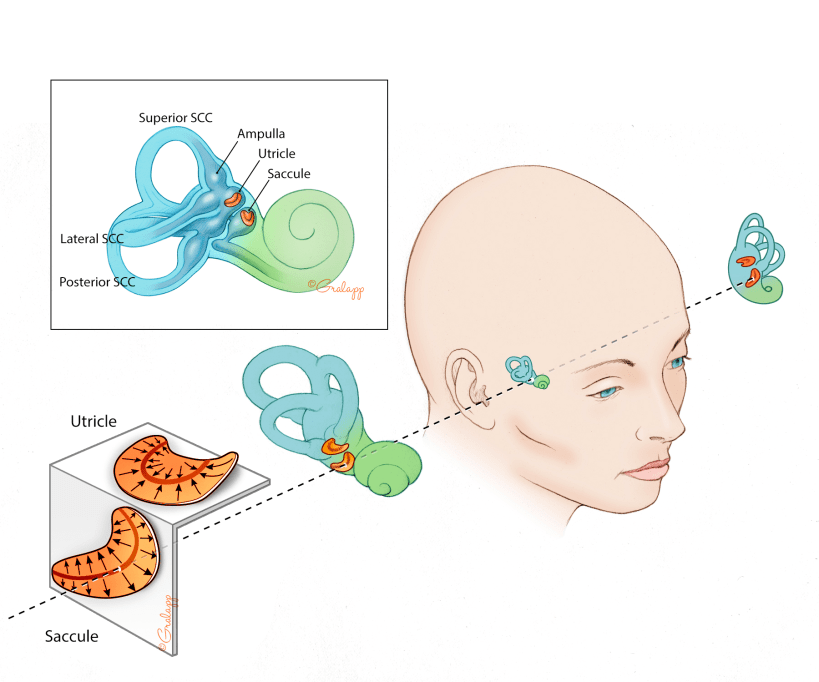
Our sense of balance is different from all our other senses. Each of our other senses has only one input: you see with your eyes, smell with your nose, hear with your ears. However, our sense of balance gets inputs from many different parts of the body. We have 5 balance organs in each ear that read your head movement in different directions. Your vision tells you where you are in space, and the feeling in the muscles and your joints coming up the spine tells you information about alignment, position and movement. All this information converges into the balance part of your brain where it integrates the information in a precise way. The brain processes this information and then send information back out. Some of that information goes to your eyes, so your gaze is stable while your head is moving. Other information gets sent to your legs so that you can stand, walk, and dance. If there is a problem anywhere in that system, the inputs, central processing, or the muscle outputs, you will experience imbalance.
There are many conditions that cause imbalance and vertigo. Vertigo is defined as any sensation that gives an illusion of motion. There are inner ear conditions that can cause imbalance, but there are many other non-ear related conditions that can affect your balance. Your doctor at Atlanta Otology can do a full evaluation of your balance issues. There are certain tests that can also give us clues to the cause of your imbalance. Many patients with imbalance will benefit from working with a special physical therapist called a vestibular therapist.
Otosclerosis
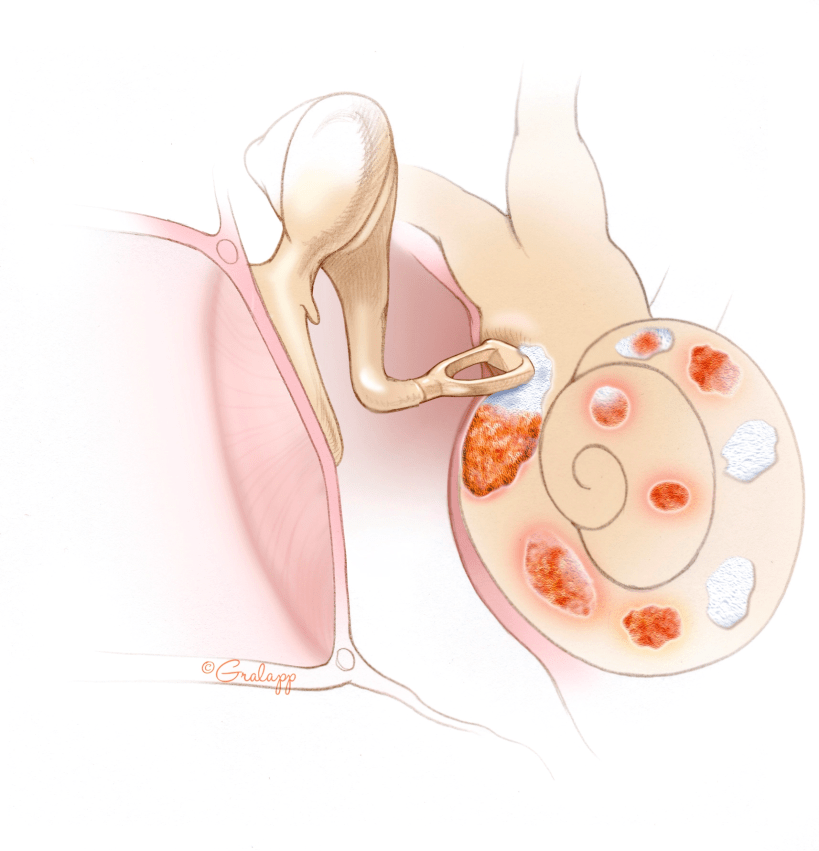
Otosclerosis is an inherited disease that affects the bones of the ear. The term “Otosclerosis” means “scarring of the ear.” Normally, the inner ear bone is a dense matured bone that does not have any regrowth. In patients with otosclerosis, however, this part of the bone begins to grow and scar in a process that evolves over many years. The scars in the ear bones eventually affect the function of the ear. The most common problem that occurs is scarring and fixation of the stapes or “stirrup” bone. This prevents the stapes bone from conducting sound from the ear drum to the inner ear, and patients develop a conductive (or mechanical-type) hearing loss. If the scarring progresses, individuals can also have a “nerve” or “inner ear” hearing loss.
Otosclerosis often present in families and more than half of people affected will have someone in the family with similar symptoms. It is more common in individuals of northern European or Indian descent, and less common in individuals of Asian or African descent. The exact cause of Otosclerosis is not known.
Symptoms of otosclerosis include hearing loss that is usually progressive over many years, tinnitus or ringing that can result from the hearing loss, and vertigo/imbalance if the otosclerosis has caused inner ear injury. A hearing test is essential in diagnosing otosclerosis. There are various ways to manage your hearing loss that results from otosclerosis, and we can discuss these at Atlanta Otology after a full evaluation and consultation.
Acoustic Neuroma/Vestibular Schwannoma
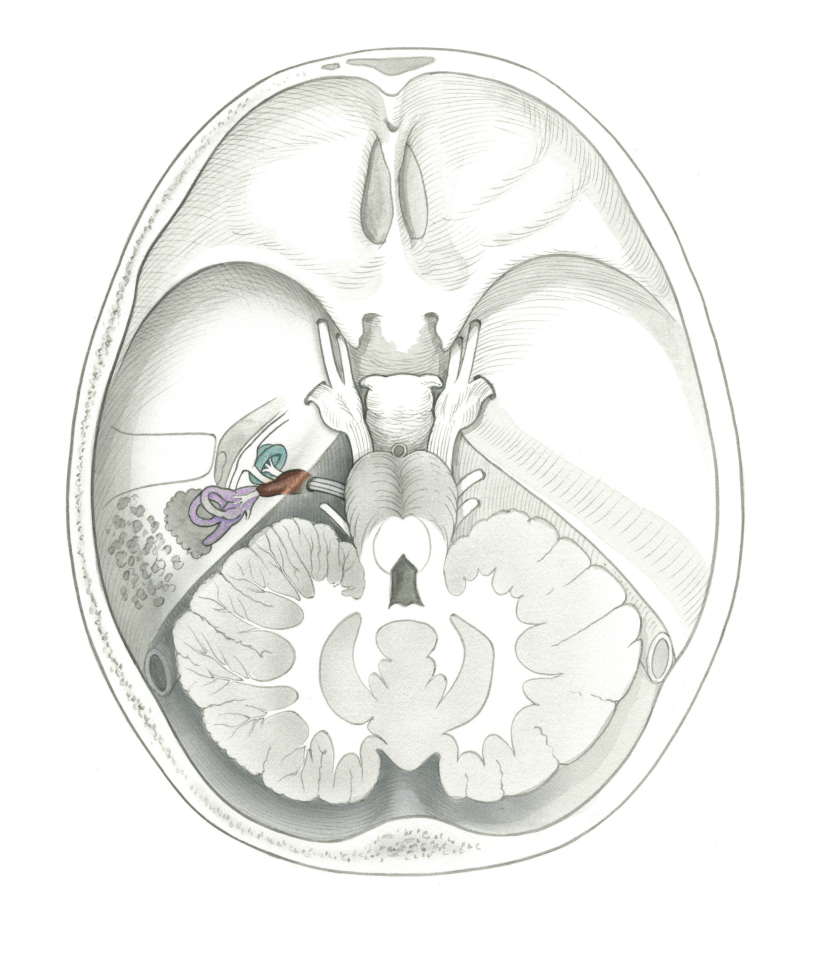
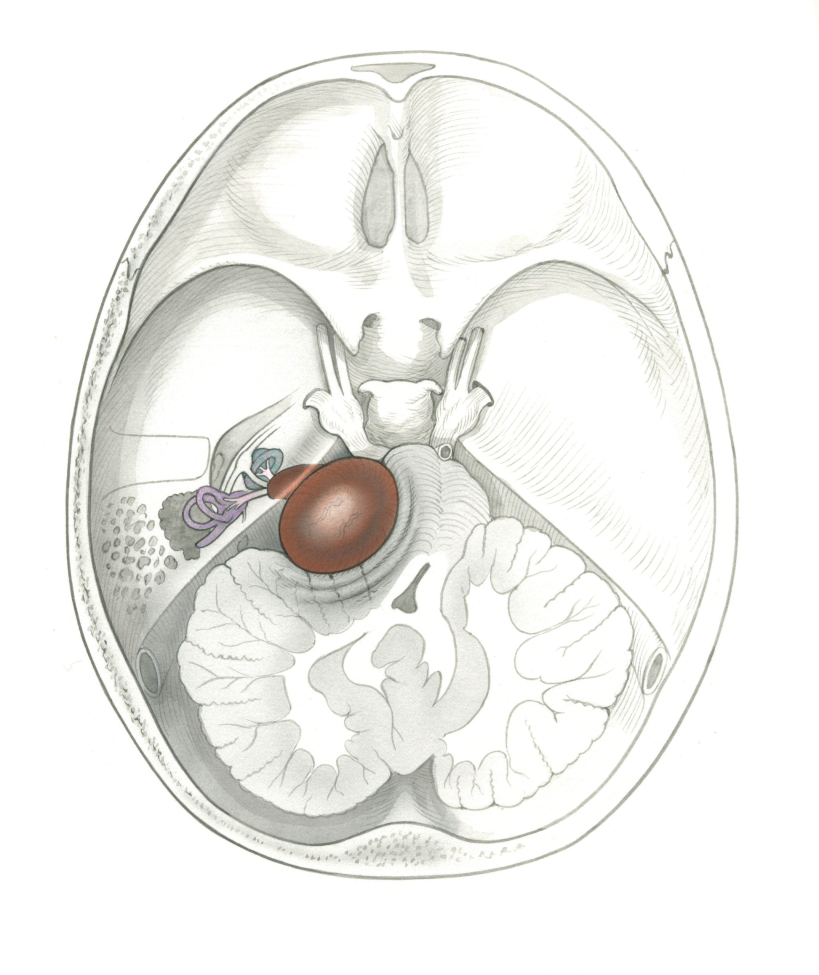
Acoustic Neuroma also known as Vestibular Schwannoma is a benign tumor of the balance (vestibular) nerve. The tumor begins inside the inner ear canal called the internal auditory canal and can expand into the brain area called the cerebello-pontine angle. Patients with acoustic neuromas typically have hearing loss, ringing or tinnitus, dizziness and imbalance. However, many patients have no symptoms. As the tumor grows larger, it can cause more severe symptoms in addition to other symptoms such as brain swelling, facial nerve weakness, and other brain complications.
The tumor is benign, but it can grow and compress important structures. The course of treatment will depend on tumor growth and size of the tumor at the time of evaluation, which will be different for each patient. Some tumors do not have any detectable growth on serial MRI scans, and these are observed. We typically consider a growing tumor to be a tumor that has >2 mm of growth on repeat MRI scans. Some tumors are very large at the time of diagnosis, and need an intervention. In rare cases, a tumor that appears to be a vestibular schwannoma can be arising from the facial nerve, which is a neighboring nerve.
Treatment options for acoustic neuromas include observation with serial MRIs, radiation, or surgical resection. The course of treatment will vary between individual patients. Your doctor at Atlanta Otology will be able to do a full evaluation and have a discussion with you about the best treatment option.
Meniere’s Disease
Meniere’s (MD) is a clinical condition that is most common in those between the ages of 40-60. MD is diagnosed when someone has two or more spontaneous attacks of vertigo each lasting anywhere from 20 minutes to 12 hours; audiogram documenting hearing loss on at least one occasion before, during or after the episode of vertigo; fluctuating ear symptoms (hearing loss, tinnitus, or fullness) in the affected ear; and other causes excluded. MD attacks are typically random, on average occurring 6-11 times per year, and can have times of remission that can last months to years.
The cause of MD is not fully understood but is thought to be due to fluid and salt imbalance in the inner ear. MD is progressive and vertigo attacks fluctuate unpredictably. Hearing loss also typically progresses. About 80% of patients will develop moderate to severe hearing loss within 15-20 years of diagnosis.
Many patients with MD are sensitive to sodium intake and do better with a sodium restrictive diet. Many also do better with diuretic therapy. This is thought to be due to a Meniere’s ear having lost its ability to tightly regulate its sodium balance within the inner ear. The sodium and salt regulation now must be controlled externally by means of diet and/or medications. A fragile Meniere’s ear may thus be intolerant of large fluctuations in sodium levels.
Although diet, lifestyle adjustments, and diuretics help the majority of MD patients control their vertigo, about 5-10% of patients unfortunately continue to have vertigo attacks. These patients may need additional treatment in the form of certain ear injections and/or surgery.
CSF Leak
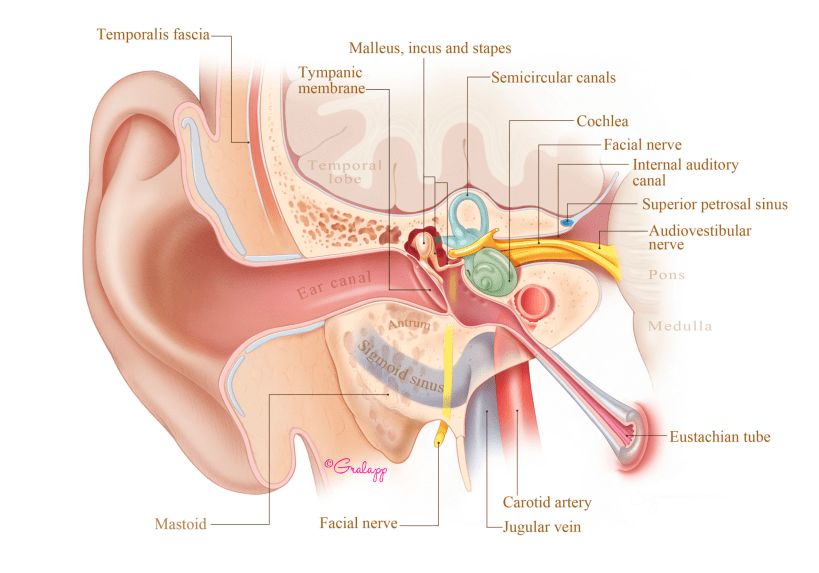
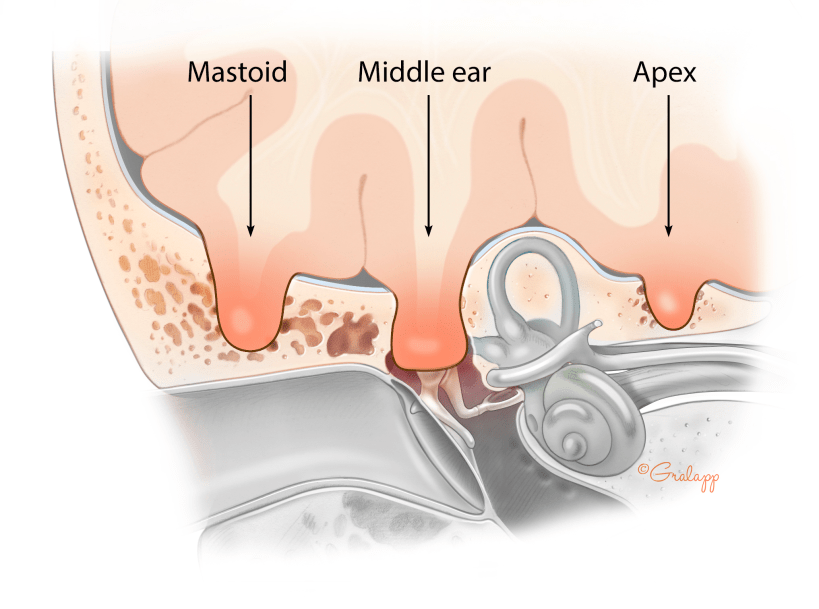
The temporal bone of the skull, which is where the ear is attached to, can sometimes develop small defects through which brain tissue or the fluid bathing the brain (called cerebrospinal fluid or CSF) can permeate into the ear. The three most common areas where this can happen are over the mastoid bone, middle ear, or the apex of the temporal bone. Brain fluid leaking into the ear is called a CSF leak. Because brain fluid is sterile while the ear is not, a CSF leak should be repaired surgically in order to avoid a brain infection. Patients with a CSF leak will often have fluid in their middle ear that will cause ear fullness and hearing loss. Sometimes this fluid will go down the eustachian tube and cause a constant post-nasal drip sensation with a salty/metallic taste. When the patient leans forward, clear fluid can also drip out of his/her nose. Although the exact reason why some people develop CSF leaks is not known, risk factors for developing this condition include being overweight, having sleep apnea, and having elevated brain pressures. Sometimes cholesteatoma can erode the skull and cause brain herniation or CSF leak. Our doctors at Atlanta Otology are experienced fixing this condition and can discuss with you the management options after a full evaluation.
Ear drum perforation
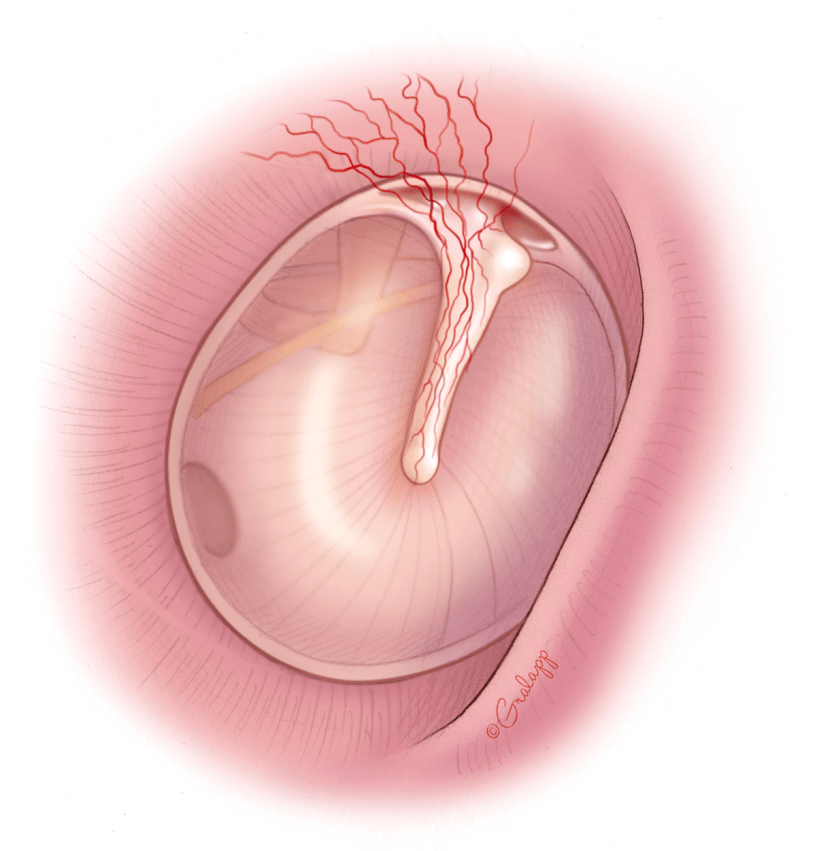
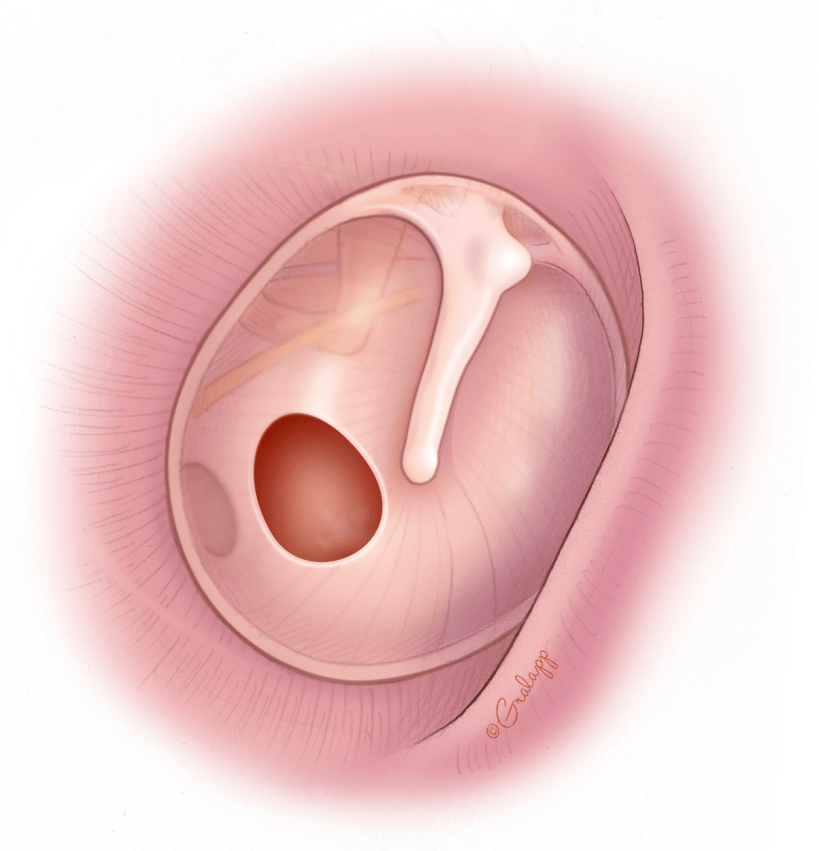
A tympanic membrane perforation, or ruptured ear drum, can result from many different causes. Trauma from a loud blast, a slap to the ear with a cupped hand, rapid changes in pressure, middle ear infections, cholesteatoma, or eustachian tube dysfunction can all lead to a hole in the ear drum. A ruptured ear drum can cause hearing loss and can make someone more susceptible to ear infections especially when exposed to water.
Smaller holes can heal on their own, while larger holes may need surgery. Perforations causing recurrent ear infections or causing significant hearing loss may be best fixed with surgery.
Eustachian Tube Dysfunction
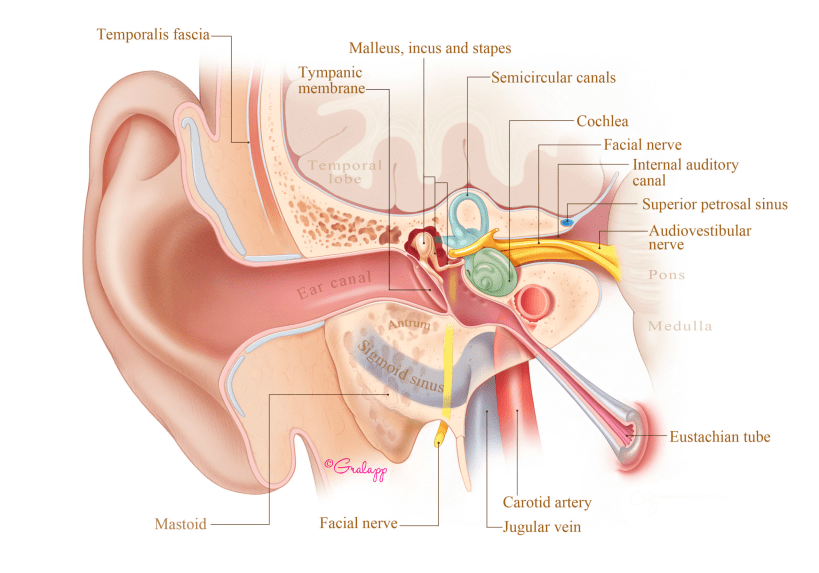
The Eustachian Tube (ET) contains a valve that is normally closed and opens intermittently, usually with swallows and yawns to allow air into the middle ear. Middle ear tissues continually use up the air and create a vacuum (negative middle ear pressure) causing the ear drum to retract until the ET opens to clear the ear and relieve the pressure. In Eustachian tube dysfunction, the opening of the valve is inadequate causing chronic negative pressure, retraction of the ear drum, and can draw fluid into the middle ear and mastoid, filling the vacuum.
Risk factors for developing chronic ET dysfunction include:
- Young child with immature ET.
- Colds, upper respiratory infections.
- Daycare.
- Exposure to smoke.
- Allergies.
- Reflux.
- Hereditary congenital problems such as cleft palate or craniofacial anomalies.
ET dysfunction will result in difficulty equalizing pressure during flying, diving or mountain driving, decreased hearing, ear infections, ear drum retractions, middle ear fluid, ear drum holes, and skin debris migrating into the middle ear and/or mastoid bone (cholesteatoma).
Patulous Eustachian Tube Disorder
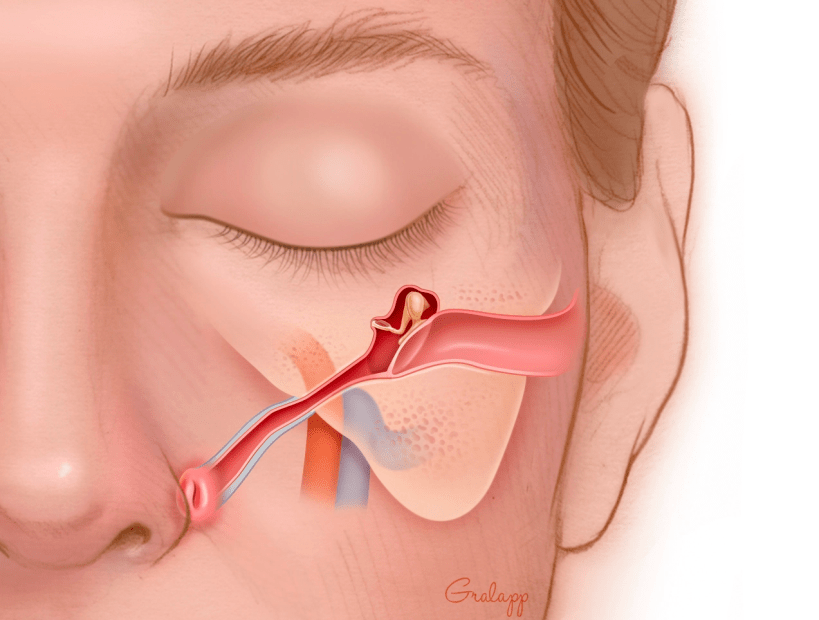
The eustachian tube is normally closed and opens briefly to clear the ears. The word ‘patulous’ comes from the word ‘patent,’ so Patulous Eustachian Tube Disorder refers to a Eustachian tube opening that is abnormally patent or open.
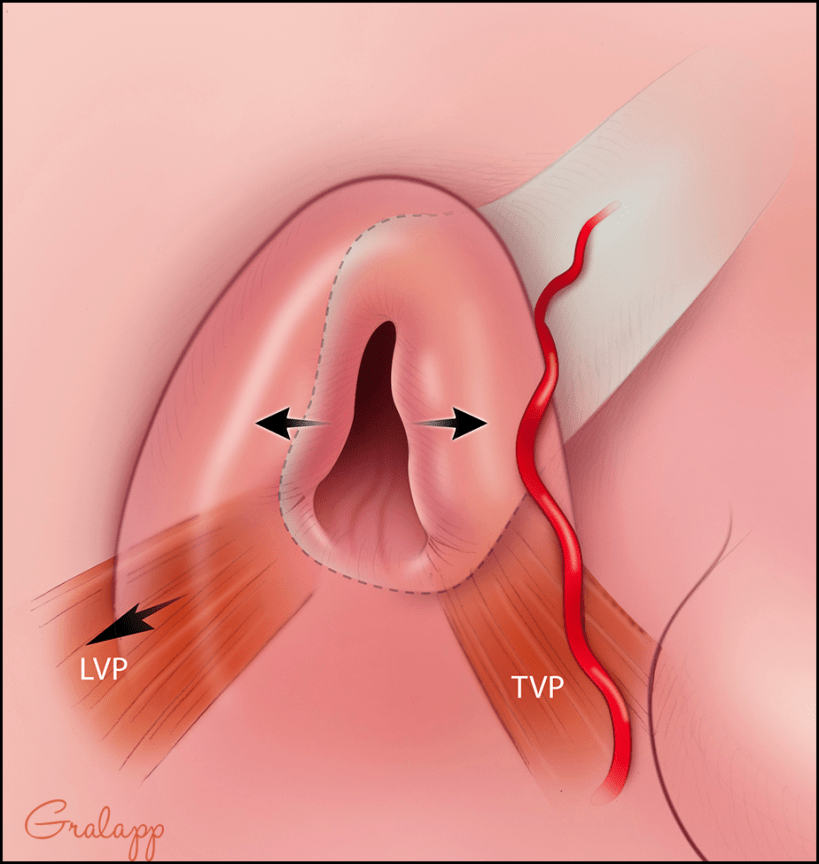
There are four main functions of the Eustachian tube which include: 1) provide ventilation to the middle ear, 2) provide a drainage pathway of middle ear fluid into the back of the nose, 3) prevent reflux of nasal contents into the ear, and 4) prevent your ear from hearing your own breathing and voice (also called autophony). Many people who have patulous eustachian tube will be bothered by hearing their own breathing and/or voice. The exact reason for why someone might develop patulous eustachian tube is not known, but rapid weight loss is a known risk factor as there is a fat pad near the eustachian tube opening called Ostman’s fat pad. Normally, the fat pad cushions the eustachian tube opening and often serves to keep the valve closed. However, with rapid weight loss, this fat pad can be lost, which in turn can cause the eustachian tube valve to remain abnormally open. Uncontrolled allergies is another risk factor since over time the nasal mucosa around the eustachian tube can atrophy as a result of chronic allergic inflammation. Patulous Eustachian Tube is diagnosed clinically through an evaluation by your doctor and a special hearing test called time-based tympanometry. There are various treatment options for treating Patulous Eustachian Tube including certain nasal drops that can engorge the nasal mucosa around the eustachian tube opening, temporary filler injections, and surgery for a more long-term solution.
Tinnitus/Ringing
Tinnitus, often described as “ringing in the ear,” is a condition in which a person perceives sound even when there is no external sound present. Tinnitus is very common and is estimated to be in at least 10% of the population.
Tinnitus is thought to result from a phantom sound that the brain generates when there is hearing loss in one or both ears. Interestingly, there has not been a correlation between the degree of hearing loss and intensity of the tinnitus. Patients most commonly describe their tinnitus as a ringing sound, but it has also been reported to sound like crickets, roaring sounds, robotic machine sounds, and others. Some people report hearing music, which has been called ‘musical tinnitus’. Tinnitus can sound louder to patients when they are stressed, lack sleep, or have poorly controlled health conditions. It is therefore important for patients with tinnitus to optimize their overall health, limit alcohol/caffeine intake, get regular sleep and exercise, and consume a healthy diet.
Some cases of tinnitus can be medication-induced. The most common medication classes associated with tinnitus are NSAIDs (such as aspirin and ibuprofen); however, there are other medications that have been associated with tinnitus.
In rare cases, tinnitus can be a symptom of a benign tumor or growth called an acoustic neuroma or vestibular schwannoma in one of the inner ear nerves. Tinnitus in these cases is typically present only on one side.
While no medical intervention can cure tinnitus at this time, tinnitus may be associated with a treatable condition. Treating the underlying cause may reduce your perception of tinnitus. For a full evaluation and hearing test, please schedule an appointment with your doctors at Atlanta Otology.
Superior Semicircular Canal Dehiscence
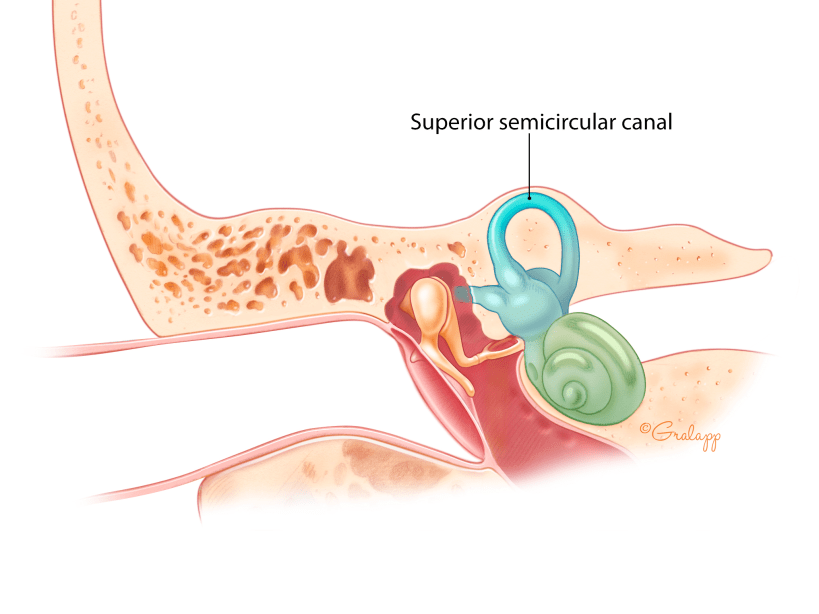
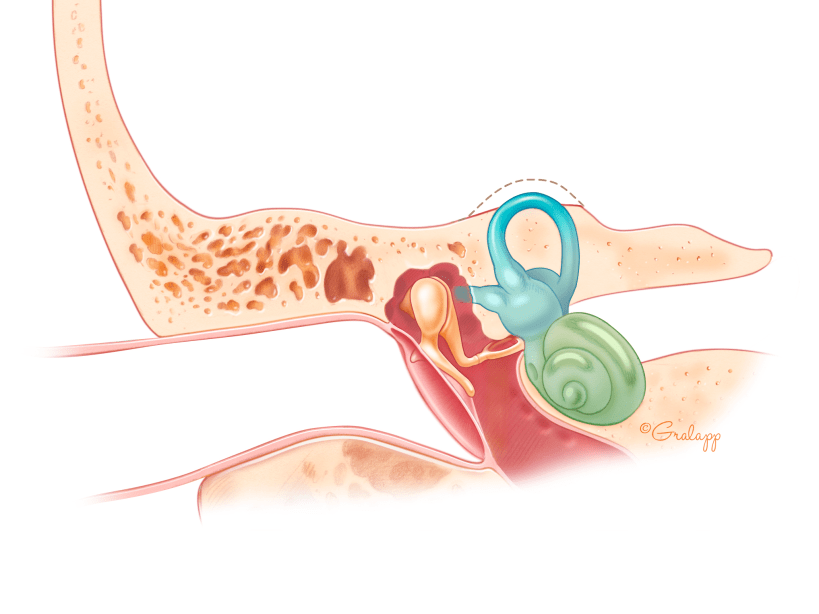
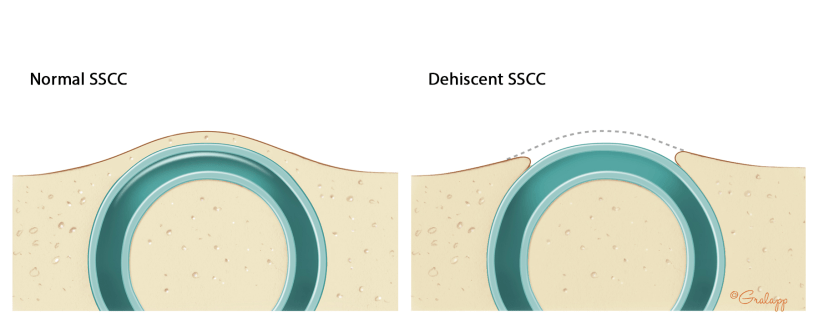
The superior semicircular canal is one of five balance organs of the inner ear, lies just under the base of the skull, and is normally covered in bone. In some patients, the bone overlying the superior semicircular canal can erode away, which can cause a syndrome called superior semicircular canal dehiscence (SSCD) syndrome. Patients with this condition can experience hearing loss and other strange symptoms such as hearing their own heart beat, having vertigo after hearing loud sounds or after bearing down, hearing their eyeball movements, or hearing their own voices. A CT scan and other balance tests can help your doctor decide whether you have SSCD. Surgical repair of the dehiscence can help improve your symptoms.
Cochlear Implantation
Cochlear Implant
What is a cochlear implant?
A cochlear implant is an electronic device that provides sound perception to patients with severe to profound sensorineural (nerve) hearing loss. Cochlear implants help in 3 primary ways: aid in lipreading, in perceiving environmental sounds, and in monitoring one’s own voice. The cochlear implant is surgically implanted and its electrode array is inserted into the hearing portion of the inner ear called the cochlea. There is also an external device that looks similar to a hearing aid that has a microphone and sound processor to collect sounds and convert them radio-wave signals. The signals travel through the skin to an antenna and receiver implanted under the skin, and the signals are then used to activate the electrode residing inside the cochlea. This, in turn, stimulates the auditory nerve with electric current and produces the perception of sound. The sound processor is individually programmed by an audiologist to best meet the needs of each patient.
Who benefits from a cochlear implant?
Patients with severe to profound sensorineural hearing loss in one or both ears may benefit from a cochlear implant. In patients with sensorineural (nerve) hearing loss, the problem is usually due to hair cell damage within the cochlea. The auditory nerve is typically still functional. A cochlear implant sends electrical signals to directly stimulate the auditory nerve by bypassing the inner ear, so patients may perceive sound with the implant despite damage to the inner ear.
Can every patient with severe to profound sensorineural hearing loss benefit from a cochlear implant?
Unfortunately, not everyone can benefit from using a cochlear implant. There are some types of sensorineural hearing loss that damage the auditory nerve, and in these cases there would be nothing that the implant can stimulate. In other types of hearing loss, there can be structural damage to the inner ear that can prevent a surgical implantation. Sometimes, it may be difficult to predict how well the implant will work on the patient. Studies have shown that duration of hearing loss and age at which the hearing loss occurred can influence the performance of the implant.
How do I know if I am a candidate?
Candidacy for cochlear implantation is determined by an otologist (ear doctor) and audiologist. The otologist will obtain a history, perform an exam, and order appropriate testing. The audiologist will evaluate your hearing by performing special hearing tests and also determine the appropriateness of amplification or hearing aids.
What is involved in having a cochlear implant operation?
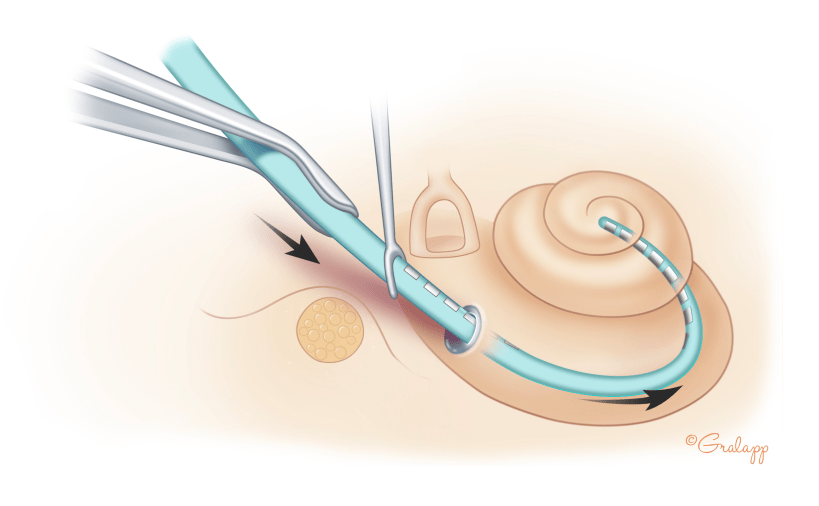
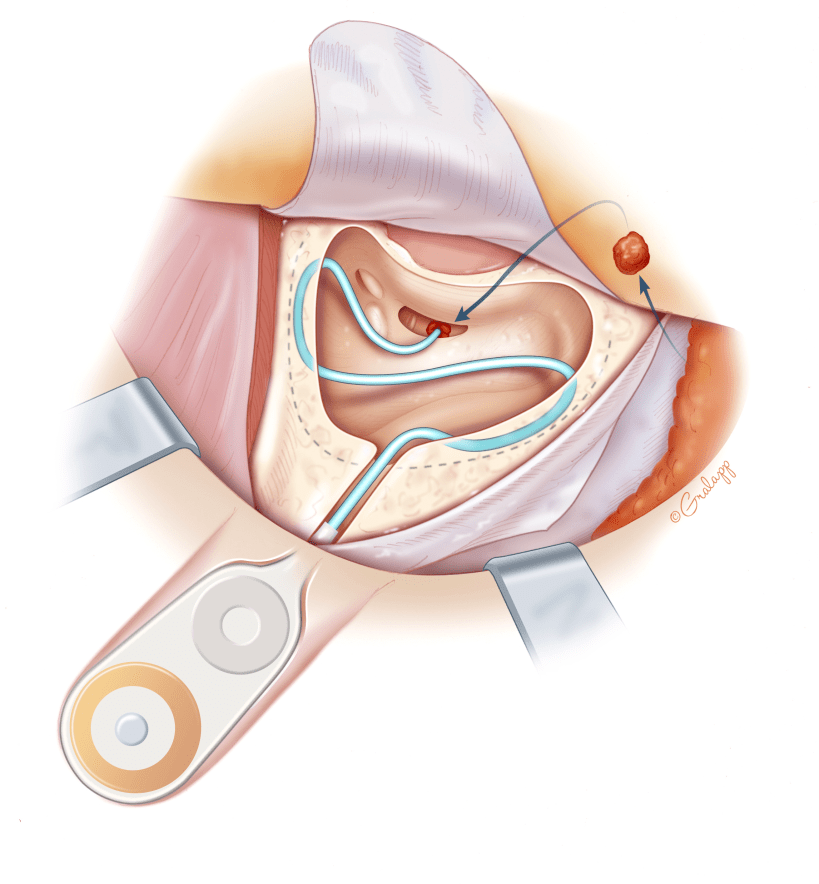
Cochlear implantation surgery is performed under general anesthesia and takes about 2 hours. An incision is made behind the ear and with the aid of an operating microscope, the surgeon will drill a portion of the bone behind the ear called the mastoid bone. A small opening is created into the cochlea, and the electrode array is threaded into the cochlea while the other implanted end is secured on the skull. This is an outpatient surgery and patients will go home the same day of surgery.
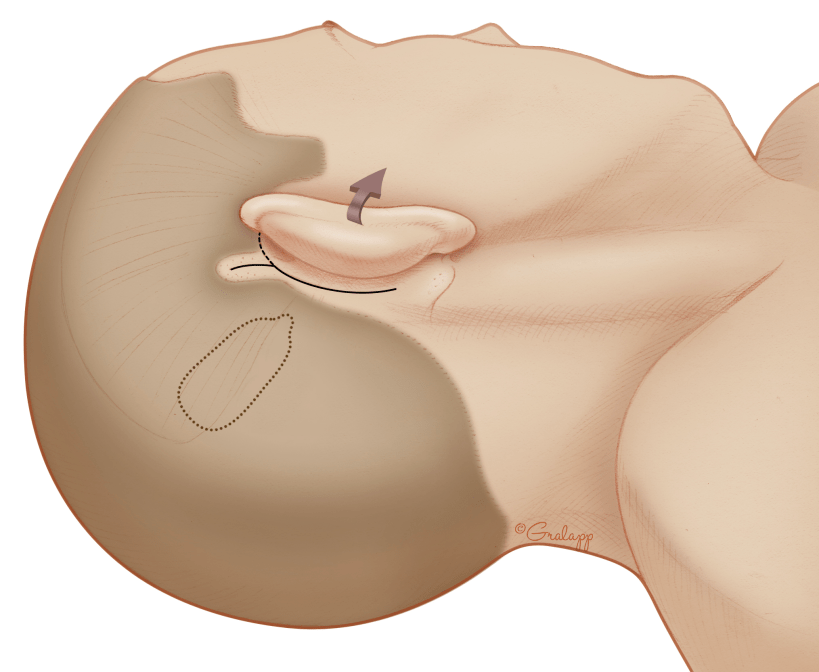
Will I hear better immediately after surgery?
Patients will not have any hearing in the operated ear immediately after surgery. The device will get activated approximately 1-3 weeks after surgery by the audiologist, which is when the device will begin working.
What does a cochlear implant sound like?
The sound generated by a cochlear implant is an electronic sound as opposed to acoustic sound that a normal ear would hear. The following YouTube clip can help us get an idea of what a cochlear implant can sound like. In the video clip, the cochlear implant recipient has normal hearing in one ear and a cochlear implant in her other ear. She tries to pick a sound clip that most closely resembles what her implant sounds like.
For more information about cochlear implants, please schedule a consultation with Atlanta Otology.
Patient Handouts (PDFs)
Understanding your hearing test
Dry Ear Precautions
Nasal Sinus Rinse Instructions
Alcohol/Vinegar Ear Flush
Steroid Side Effects
Precautions for patients with unilateral hearing
Eustachian Tube Dysfunction
Patulous Eustachian Tube
Vestibular Disorders - An Overview
Laboratory Tests for Dizzy Patients
Coping With a Vestibular Disorder
Vestibular Migraine
Vestibular Neuritis/Labyrinthitis
Cervicogenic Dizziness
Mal de Debarquement
Concussion and dizziness
Persistent Postural Perceptual Dizziness (PPPD)
Tinnitus/Ringing
Oral Fluoroquinolone Information
Eye Care - Facial Weakness
Cholesteatoma
CWU vs CWD
Cochlear Implant Information
Tests for Pediatric Hearing Loss
Vaccines for Cochlear Implantation and CSF Leak Patients
Sudden Sensorineural Hearing Loss Literature
Meniere’s Disease Handouts
FM Transmitter
Post-Operative Instructions (PDFs)
Tympanoplasty and Mastoidectomy
Stapedectomy and Transcanal Procedures
Cochlear Implantation
Middle Fossa Craniotomy
Eustachian Tube Procedure
Myringotomy and Tympanostomy Tubes
Surgery Photo and Video Release Form